Introduction
Antimicrobial resistance (AMR) concern is threatening worldwide and raising concerns for health security about how to cure the infections and diseases in a safe manner through contemporary medical therapies (1). According to the World Health Organization (WHO), AMR is considered one of the biggest risks that global public health is facing nowadays if no heed is paid to the current trends, it can lead to disastrous outcomes (2). Pakistan has a population of over 240 million; it is also a lower middle-income nation that faces unique hurdles against AMR due to socioeconomic issues, healthcare system constraints, and regulatory deficiencies (3). The increased use of antibiotics, poor diagnostic facilities, and wide socioeconomic gaps will impact the health care sector and lead to AMR spread (4). The AMR is causing a burden globally, as the trend of fatality rate is around 700,000 AMR-attributable fatalities per year, in reference to the recent comprehensive assessments (5). Household expenses are increased by AMR. Poorer people suffer more because of the suffering and early deaths it causes. It hinders economic progress and lowers community productivity. Early death and disability are caused by a decrease in labor supply and an increase in healthcare demand (6).
Literature review
Antimicrobial resistance (AMR) is one of the increasing threats to global health. The risk in surgeries and medical procedures, which includes organ transplant, heart surgeries, cancer therapies, and other surgical operations, has major health risks due to hospital-acquired AMR. Patients experience vast issues due to longer hospital stays, and very less options for treatments are available, as with time antibiotics lose their effectiveness; all these concerns raise the burden on the healthcare system. AMR has vital societal and economic implications in addition to its influence on clinical outcomes. AMR is directly related to longer hospital stays; as the patients’ stay becomes longer, the medical cost also increases, and the healthcare resources are used more in both developed and developing countries. AMR decreases the productivity of workers, and it also puts pressure on national economies at the societal level. As estimated, it impacts the economic growth, which is a major worldwide health issue. To properly handle this crisis, global efforts are required to overcome these major problems. We require strong surveillance systems to detect, monitor, and respond quickly to resistance trends and robust antimicrobial stewardship programs, which are essential for ensuring the proper and sensible use of antibiotics. The effective approach of One Health shows the link between human, animal, and environmental health. This acknowledges that the use of antibiotics in the environment and in agriculture directly contributes to the development of resistance in human populations. In short, AMR is a complicated, diverse issue. As the resistance is rising, it will continue to hinder medical advancement, deteriorate health systems, and place increasing stress on future generations until further actions are taken (7).
Aims and objectives
The following goals guided the creation of this study:
• To compile worldwide patterns in AMR from 2020 to 2025.
• To assess and outline the state of AMR.
• To illustrate the parallels and discrepancies between Pakistan’s AMR trends and worldwide trends.
• To evaluate the financial and medical costs associated with AMR in Pakistan.
• To point out areas for improvement in stewardship, policy, and surveillance and offer recommendations for the future.
Methodology
Study design
This study was conducted as a systematic review and meta-analysis to summarize the latest data on AMR in Pakistan and compare it to global trends between 2020 and 2025.
Study population and sampling frame
The “population” of studies, surveillance reports, and datasets that examined the mechanisms of antibiotic resistance and the prevalence of AMR in human clinical samples. Studies were carried out at the national level in Pakistan as well as international reports. No direct patient recruitment was carried out. Instead, a systematic sampling of published literature was carried out via reference screening and database searches.
Search strategy
The databases PubMed, Scopus, Web of Science, and Google Scholar were used in a methodical search. Articles published between January 2020 and June 2025 were included in the search. “Antimicrobial resistance” OR “AMR” AND “Pakistan” OR “global trends” AND “GLASS” OR “One Health” OR “ESBL” OR “carbapenem resistance” were among the keywords and Boolean operators utilized. To find more pertinent articles, the reference lists of the included research and official reports from the Global Antimicrobial Resistance and Use Surveillance System (GLASS) and the WHO were also searched.
Eligibility criteria
Inclusion criteria
• Research on the prevalence of AMR, resistance mechanisms, or patterns of antibiotic use.
• Articles that offer information particular to Pakistan or on a worldwide scale.
• Systematic reviews, surveillance reports, or peer-reviewed observational research.
• Printed in English from 2020 to 2025.
Exclusion criteria
• Editorials, conference papers, or case reports that don’t include primary data.
• Research that has no obvious connection to human health and only looks at environmental or veterinary materials.
• Incomplete or duplicate reports that lack adequate methodological information.
Sample size consideration
The number of eligible studies included in this meta-analysis determined the sample size, despite the fact that no patients were personally recruited. To enable pooled estimates across research, the patient/sample population size from each study was retrieved and presented.
Data extraction and management
Reviewers used a standardized data collection sheet to independently extract this data. Publication year, study design, geographic location, study population, bacterial species, sample size, antibiotic susceptibility patterns, and resistance rates were among the data that were extracted.
Statistical analysis
Instead of doing a primary data study, this research was carried out as a systematic research analysis. There were no new mathematical models or statistical tests used. A descriptive comparison of data taken from official surveillance reports and published studies was used instead.
• The findings were categorized thematically, covering bacterial species, antibiotic consumption patterns, resistance mechanisms, and worldwide versus Pakistan-specific trends.
• Reported prevalence rates and resistance percentages were documented precisely as they were in the original sources.
• The results of several research studies that looked at the same parameter were compared side by side to find trends, variances, and consistent findings.
• After that, the data were narratively synthesized to show the main parallels and divergences between Pakistan and the global AMR trends of 2020–2025.
Duration of study
The search, screening, data extraction, and analysis steps of the procedure were carried out from July 2024 to August 2025.
Ethical considerations
This study was carried out as a meta-analysis and systematic review. There were no new human or animal participants in this study. Every piece of information was taken from publicly accessible surveillance reports and previously published peer-reviewed research. Therefore, ethical clearance was not necessary.
Global AMR trends and burden
Worldwide resistance patterns
Global surveillance data shows that AMR has grown at a never-before-seen rate in all major disease groups and geographical locations. The most recent comprehensive analysis, which spans 2020–2025, reveals concerning trends in illnesses associated with both the general public and healthcare. Sub-Saharan Africa bears the largest burden of AMR-associated mortality in 2023, with approximately 1.4 million deaths, followed by South Asia with 980,000 deaths. This highlights the disproportionate impact on regions with few resources. AMR mortality is still highest in low- and middle-income areas, as Table 1 illustrates, highlighting the critical need for improved stewardship and surveillance (8).
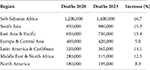
Table 1. Global AMR burden by region (2020–2023) (8).
Key pathogen-antibiotic combinations
The worldwide burden of AMR has increased dramatically, affecting all regions, but low- and middle-income countries are disproportionately impacted due to their insufficient healthcare, weak laboratory capacity, and surveillance systems. A number of pathogen-antibiotic combinations have become specific issues (9):
Critical priority pathogens: – Carbapenem-resistant
Acinetobacter baumannii – Carbapenem-resistant
Pseudomonas aeruginosa – Carbapenem-resistant Enterobacteriaceae
High priority pathogens: – Vancomycin-resistant
Enterococcus faecium – Methicillin-resistant
Staphylococcus aureus (MRSA) – Fluoroquinolone-resistant Campylobacter spp.
Economic impact and healthcare burden
Beyond just direct medical costs, AMR has significant economic repercussions, such as decreased productivity, extended hospital stays, and the need for more expensive alternative therapies. Global estimates currently place the yearly expenses between $100 and $150 billion, and without effective intervention, projections show exponential increases. Higher rates of treatment failure, longer hospital admissions, and the requirement for more intensive care treatments are all signs of the healthcare burden. Between 2020 and 2025, the AMR research timetable identifies important worldwide initiatives and research goals, including financing pledges, behavior change research, and pandemic preparedness (Figure 1).
Figure 1. AMR research timeline and key milestones (2020–2025). This figure illustrates the progression of major AMR research developments, policy implementations, and surveillance milestones from 2020 to 2025, including the expansion of GLASS networks, development of national action plans (NAPs), and key breakthrough research findings.
AMR situation in Pakistan: current status and challenges
National surveillance data and resistance patterns
Participation by Pakistan in international monitoring networks, especially GLASS, has yielded important information about patterns of domestic opposition. Nonetheless, there are still large gaps in data from primary healthcare settings and rural areas, and surveillance coverage is still restricted. Data that is currently available shows alarming patterns in a number of disease groupings (10):
Gram-negative bacteria: E. coli and Klebsiella spp. are becoming more resistant to carbapenem and polymyxins throughout Africa. E. coli is more than 50% resistant to cephalosporins and fluoroquinolones, while Klebsiella is more than 25% resistant to carbapenem. (11).
Gram-positive microorganisms: The frequency of MRSA varies greatly from hospital to hospital (15–60%). Enterococci resistant to vancomycin are appearing in tertiary care facilities. Concerning penicillin and macrolide resistance in Streptococcus pneumoniae (12).
Antibiotic consumption patterns
Over the past 10 years, Pakistan’s national consumption of antibiotics has increased by an estimated 65% due to a number of variables, including patient demand, improper prescribing practices, and over-the-counter availability. With an antibiotic use prevalence of 82.1% and a hospital culture-guided prescribing rate of only 2%, pediatric point-prevalence surveys show especially alarming trends (13).
Essential Consumption Factors: Antibiotics available over-the-counter; limited diagnostic capabilities resulting in empirical medication; and incomplete treatment regimens because of financial limitations. The use of antibiotics in agriculture and veterinary medicine; the absence of systems to enforce prescriptions.
Healthcare system challenges
The following structural issues with Pakistan’s healthcare system contribute to the emergence and spread of AMR:
Infrastructure limitations: Limitations of the Infrastructure: Insufficient lab space for sensitivity and culture testing, restricted availability of quick diagnostic instruments, inadequate methods to prevent and control infections, and overcrowding in medical institutions makes transmission easier.
Human resource constraints: Limited training on antimicrobial stewardship – Shortage of clinical microbiologists and infectious disease specialists – Inadequate continuing education programs – Poor awareness among healthcare workers.
Mechanisms of antimicrobial resistance
Enzymatic inactivation
One of the most important resistance mechanisms in clinical practice is the generation of enzymes that render antimicrobial drugs inactive. With high prevalence rates among Enterobacteriaceae, carbapenemases and extended-spectrum beta-lactamases (ESBLs) have become especially problematic in Pakistan (13).
Key enzyme families: ESBLs: Cefotaximase-Munich (CTX-M), sulfhydryl variable (SHV), and temoniera (TEM) Carbapenemases: Klebsiella pneumoniae carbapenemase (KPC), New Delhi metallo-β-lactamase (NDM), imipenemase metallo-β-lactamase (IMP), oxacillinase (OXA)-48-like, and verona integron-encoded metallo-β-lactamase (VIM) Change-causing enzymes for aminoglycosides chloramphenicol acetyltransferases.
Modification of the target
Antimicrobial target site alterations that reduce drug binding affinity lead to resistance. This procedure is particularly important for: fluoroquinolone-resistant DNA gyrase and topoisomerase IV mutations.
• Penicillin-binding protein alterations in S. aureus (MRSA).
• Methylation of 16S rRNA in resistance to aminoglycosides.
• Resistance to vancomycin due to alteration of peptidoglycan precursors
Reduced permeability and active efflux
The multidrug resistance patterns seen in Pakistan are largely caused by modifications in the permeability of the bacterial cell membrane and increased efflux pump activity:
Permeability changes: Porin loss or alteration in Enterobacteriaceae Bacteria that are Gram-negative Composition of lipopolysaccharides (14).
Efflux pump systems: resistance-nodulation-division (efflux pump family) (RND) family pumps in gram-negative bacteria (15) S. aureus ABC transporters major facilitator superfamily (efflux pump family) (MFS) pumps in a variety of species.
Biofilm formation
Biofilm-associated disorders provide special challenges in Pakistani healthcare settings since they result in chronic infections and treatment failures. Biofilms provide protection against antibiotics in a number of ways (16).
Decreased immune system evasion, altered metabolic states of implanted bacteria, facilitated horizontal gene transfer, and decreased penetration of antimicrobial agents (16).
Surveillance systems and data quality
Global surveillance networks
Pakistan’s participation in international surveillance networks, particularly WHO GLASS, has enhanced understanding of national resistance patterns. However, data quality and coverage remain significant challenges (10):
GLASS participation: few participating laboratories – Attention on tertiary care centers – Inadequate illustration of rural areas – Standardization challenges across laboratories.
National surveillance infrastructure
Pakistan’s national surveillance system faces multiple challenges that limit its effectiveness in monitoring AMR trends:
System limitations: Fragmented data collection mechanisms – few capacities laboratory for quality surveillance – Insufficient data management systems – Poor unification between public and private sectors.
Quality assurance issues: Inconsistent laboratory methods – Limited external quality assessment participation – Inadequate staff training – Resource constraints affecting testing quality.
Data gaps and limitations
Significant gaps exist in Pakistan’s AMR surveillance data, potentially introducing bias toward urban, tertiary care settings. Standardization of laboratory methods and resistance definitions may vary between studies, affecting comparability. The economic impact analysis is limited by the scarcity of comprehensive cost-effectiveness studies specific to the Pakistani context (17).
Policy framework and national action plan
Pakistan’s national action plan on AMR
In line with WHO’s Global Action Plan, Pakistan created its National Action Plan (NAP) on AMR in 2017. However, there are several obstacles to implementation:
NAP goals: The NAP on AMR aims to reduce infection risks through better biosecurity, hygiene, and vaccination programs, ensure responsible and prudent use of antimicrobials in human medicine and livestock production, promote long-term investment in sustainable alternatives like vaccines, probiotics, and phytochemicals, and increase awareness and knowledge of AMR across human, animal, and environmental health sectors. In line with Sustainable Development Goals 3 (Good Health and Well-Being), 12 (Responsible Consumption and Production), and 15 (Life on Land), these goals are incorporated into the One Health framework (18).
Implementation difficulties: Poor inter-sectoral coordination, a lack of finance, and inadequate monitoring and evaluation systems—Inadequate provincial political commitment (19).
Regulatory framework
The antimicrobial regulatory framework in Pakistan has to be significantly strengthened:
Current rules: The 1976 Drug Act and the 1978 Drug Regulations, National Drug Policy 2018, antimicrobial import and manufacturing licenses, and inadequate enforcement measures.
Regulatory omissions: Prescription medicines that are available over-the-counter, inadequate quality control of imported antimicrobials, little regulation of the use of antibiotics in veterinary medicine, and lax penalties for regulatory infractions.
Antimicrobial stewardship programs
Pakistan’s adoption of antimicrobial stewardship is still lacking, with notable gaps in the public and private healthcare systems:
Present situation: A small number of hospitals have official stewardship initiatives. Poor monitoring of antibiotic use, inadequate prescriber education, and a lack of clinical chemist engagement (20).
Implementation obstacles: Lack of qualified staff, inadequate institutional support, restricted ability to diagnose, and financial problems in environments with limited resources.
Economic burden and healthcare costs
Direct healthcare costs
Although thorough cost estimates are still scarce, there are several ways that AMR’s economic burden appears in Pakistan:
Rising medical expenses: Longer hospital stays and more costly second-line therapies, extra diagnostic tests a rise in the need for critical care (21).
Costs of treatment failure: Recurrent hospital stays, needs for long-term care, needs for palliative care (22).
Indirect economic impact
Antimicrobial resistance (AMR) has substantial indirect economic consequences in addition to direct healthcare costs:
Losses in productivity: Prolonged period of illness, the premature death rate (23), the strain of caregiving (24), and decreased involvement in the labor force (25).
Impact on the healthcare system: A diminished ability to do elective treatments (26), enhanced standards for infection control (27), and the strain on infrastructure (28).
Projected economic burden
Pakistan risks increasing economic implications from AMR in the absence of effective intervention. According to conservative estimates, if current trends continue, GDP losses might reach 2–3% by 2030, with vulnerable communities bearing a disproportionate amount of the burden.
One health approach and environmental factors
Human-animal-environment interface
Environmental factors and agricultural practices in Pakistan have a major impact on the emergence and spread of AMR:
Agricultural antibiotic use: Livestock growth promotion, aquaculture disease prevention, inadequate veterinarian supervision, and food product contamination.
Environmental contamination: Waste from pharmaceutical manufacture, discharge of hospital effluent, and runoff from agriculture and urban wastewater systems.
Food safety and AMR (29)
In Pakistan, one important route for the spread of AMR is the food chain:
Contamination sources: Production of poultry and livestock, aquaculture methods, food processing facilities, and retail and distribution networks.
Risk factors: Inadequate cold chain infrastructure, inadequate personal hygiene, and inadequate laws pertaining to food safety.
Environmental surveillance
Pakistan still lacks adequate environmental surveillance for AMR, which is a crucial knowledge gap in resistance ecology (9):
Priority areas: Wastewater from hospitals, manufacturing facilities for pharmaceuticals, urban water systems, and agricultural settings.
In order to prevent AMR, the One Health paradigm stresses the integration of environmental, animal, and human health through integrated actions such as waste management, surveillance, and responsible antibiotic use (Figure 2).
Figure 2. One Health approach to AMR intervention integration. The link of the human, animal, and environmental health sectors in AMR prevention and control is shown in this picture, which also spotlights the importance of coordinated efforts across all three domains and how interventions in one can affect the others.
Antimicrobial stewardship and infection prevention
Hospital-based stewardship programs
Despite several obstacles, the implementation of antimicrobial stewardship programs in Pakistani hospitals is an essential intervention (30):
Core components: Guidelines for prescribing antibiotics (31), pre-authorization specifications, prospective evaluation and comments, and interventions in education (32).
Implementation Barriers: Clinical pharmaceutical services are limited (33), poor diagnostic assistance, prescriber resistance (34), and limitations on resources.
Community-level interventions
Interventions for community-based stewardship are crucial in combating improper use of antibiotics:
Key strategies: Campaigns for public awareness (35), interventions based on pharmaceuticals (36), and programs for community health workers and training for primary healthcare providers.
Challenges: Low levels of health literacy, cultural perspectives on antibiotics, financial obstacles to receiving the right care, and inadequate enforcement of regulations.
Infection prevention and control
Improving infection prevention and control (IPC) strategies is essential to lowering the spread of AMR:
Priority interventions: Programs for hand hygiene (37), procedures for cleaning the environment (38), precautions for isolation, and monitoring of infections linked to healthcare.
System requirements: Programs for IPC training (39), sufficient numbers of employees, enhancements to the infrastructure, and mechanisms for ensuring quality.
Laboratory capacity and diagnostic challenges
Current laboratory infrastructure
Pakistan’s laboratory capability for clinical management and AMR surveillance is still insufficient:
Limitations on capacity: A small number of authorized labs, inadequate supplies and equipment, a lack of technological know-how, and inadequate programs for quality assurance (40).
Geographical differences: Concentration in cities, restricted access to laboratories in remote places, difficulties with transportation, and barriers to communication.
Gaps in diagnostic technology
Modern diagnostic technology access is still restricted, which has an impact on clinical care and surveillance:
Needs for technology: Systems for automated susceptibility testing, quick diagnostic tools, capabilities for molecular diagnostics, and options for point-of-care testing.
Execution challenges: Expensive equipment and requirements for maintenance and requires training the supply chains for reagents.
Quality assurance and standardization
There must be methodical changes made to Pakistan’s laboratory network to guarantee quality and uniformity:
Measures of quality: Programs for external quality assessment, standardized protocols for operations, participation in proficiency testing, and procedures for accreditation.
Capacity developing requirements: Programs for technical training, support for equipment maintenance, systems for managing quality, and capabilities for data management.
Future strategies and recommendations
Strengthening surveillance systems
Effective AMR response requires a comprehensive strengthening of the surveillance system:
Priority tasks: Increase participation in GLASS, create national guidelines for surveillance, and combine data from the public and private sectors and create regional networks for surveillance.
Integration of technology: Electronic medical records, information systems for laboratories and platforms for sharing data in real time, and mechanisms for automated reporting.
Policy and regulatory reforms
To effectively combat AMR, significant legislative and regulatory changes are required:
Priorities for legislation: Antimicrobials are only available with a prescription, veterinary antibiotic laws, requirements for quality control, and enhancement of penalties for infractions.
Mechanisms of implementation: Platforms for interagency coordination, systems for monitoring and evaluating performance, procedures for engaging stakeholders, and tactics for mobilizing resources.
Capacity building and education
For a sustainable AMR response, comprehensive capacity building in all sectors is essential:
Healthcare workforce: Training in antimicrobial stewardship, education on infection prevention, and capacity building for laboratories’ ongoing professional growth.
Education of the Public: Campaigns for community awareness, programs for education in schools, strategies for engaging the media, and interventions for behavior change.
Priorities for research and innovation
Research and innovation are essential for developing context-appropriate solutions:
Priority research areas: – Economic impact assessments – Implementation research on stewardship interventions (41).
Innovation needs: – Rapid diagnostic development – Novel therapeutic approaches – Digital health solutions – Implementation tools and resources.
International collaboration and support
Global partnerships
International cooperation and assistance are beneficial to Pakistan’s AMR response:
Important collaborations: WHO technical support, financed by the World Bank Agreements for bilateral cooperation, and collaborations in academic research.
Areas of support: Building technical competence and providing financial support, sharing of knowledge, and transfer of technology.
Collaboration in the region
In South Asia, regional collaboration is crucial to tackling cross-border AMR issues:
Cooperation prospects: Coordinated regulatory standards and shared surveillance systems and coordinated policy responses and collaborative research projects.
Regional difficulties: Tensions in politics, inequalities in income, disparities in regulations, and inadequate institutional capability.
Results
Antimicrobial resistance (AMR) rates have significantly increased globally, and in Pakistan specifically, according to the analysis’s findings for the years 2020–2025. Majorly two resistances are increased, which are fluoroquinolone and third-generation cephalosporin resistance. In Pakistan, a major variety of bacterial infections, such as K. pneumoniae and E. coli, show resistance to these antibiotics.
Discussion
The AMR is particularly increasing in Pakistan; it shows concerns for the urgent need for comprehensive strategies that incorporate the One Health paradigm, surveillance, and responsible antibiotic use. The One Health shows the interconnected health problems that impact humans, animals, and the environment, which is a synergistic approach to AMR control. The socioeconomic and healthcare problems in Pakistan, such as the more use of antibiotics and inadequate diagnostic facilities lead to a higher mortality rate. The lab networks and resources should be strengthened, and the protocol of hygiene and sanitization should be maintained to overcome the AMR initially.
Conclusions
The prevalence rate of AMR in Pakistan is higher than the global average for several pathogen-antibiotic combinations, which presents an important and growing public health risk. Several important conclusions are drawn from the analysis:
• Escalating burden: Pakistan is facing an increasing AMR burden that is in line with global trends, but regional challenges are exacerbated by limitations in the healthcare and socioeconomic systems.
• Surveillance gaps: The significant gaps in surveillance coverage and data quality make it challenging to effectively track trends and guide responses.
• Implementation challenges: Despite having a NAP, there are several challenges to its implementation, including inadequate funding, a lack of coordination, and a lack of enforcement of regulations.
• Economic impact: AMR has a significant and increasing financial burden, and without effective action, forecasts show dire repercussions for Pakistan’s healthcare system and economy.
• Multisectoral nature: The One Health approach tackles the environmental, animal, and human elements that affect the spread of resistance and is required to combat AMR in Pakistan.
To counter the rising tide of resistance, antimicrobial stewardship programs, improved surveillance systems, and legislative reforms must be implemented immediately. For Pakistan’s public health security, prompt, coordinated intervention is essential because the window for effective action is closing.
Future research directions
Several areas warrant priority attention for future research in Pakistan:
• Economic modelling: The creation of thorough economic models that account for direct medical expenses, lost productivity, and wider economic effects in order to fully assess the burden of AMR.
• Implementation research: Studies on practical, affordable stewardship initiatives tailored to environments with limited resources.
• One health surveillance: Extensive surveillance studies that look at the intersection of environmental reservoirs and food chain contamination with human, animal, and environmental resistance.
• Social and behavioral research: To guide focused treatments, it is important to comprehend patient expectations, prescribing practices, and cultural elements affecting antibiotic use.
• Diagnostic innovation: Creation and assessment of quick, reasonably priced diagnostic instruments appropriate for Pakistani medical environments.
• Policy research: Assessing the application of policies and regulatory actions to determine the best governance strategies.
Author contributions
AA: Conceptualization, Data collection, Meta-analysis, Writing – original draft. SR: Literature review, Methodology refinement, Writing – review and editing. Both authors: Review and approval of the final version, Accountability for all aspects of the work.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Acknowledgments
The authors thank the public health experts, academics, and doctors whose publications and surveillance activities enabled this thorough analysis. The WHO GLASS network and country surveillance teams deserve special commendation for their continued dedication to AMR reporting and monitoring.
We also thank Pakistani public health officials, laboratory staff, and healthcare professionals who, in spite of severe system and resource restrictions, never stop working to solve AMR issues.
Conflicts of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
1. Ifedinezi OV, Nnaji ND, Anumudu CK, Ekwueme CT, Uhegwu CC, Ihenetu FC , et al. Environmental antimicrobial resistance: implications for food safety and public health. Antibiotics. (2024) 13(11):1087.
2. Rony MKK, Sharmi PD, Alamgir HM. Addressing antimicrobial resistance in low and middle-income countries: overcoming challenges and implementing effective strategies. Environ Sci Pollut Res. (2023) 30(45):101896–1902.
3. Saleem Z, Godman B, Azhar F, Kalungia AC, Fadare J, Opanga S , et al. Progress on the national action plan of Pakistan on antimicrobial resistance (AMR): a narrative review and the implications. Expert Rev Anti Infect Ther. (2022) 20(1):71–93.
4. Puvača N, Tankosić JV, Ignjatijević S, Carić M, Prodanović R. Antimicrobial resistance in the environment: review of the selected resistance drivers and public health concerns. J Agron Technol Eng Manag. (2022) 5(5):793–802.
5. Adebisi YA, Ogunkola IO. The global antimicrobial resistance response effort must not exclude marginalised populations. Trop Med Health. (2023) 51(1):33. doi: 10.1186/s41182-023-00524-w
6. Jit M, Ng DHL, Luangasanatip N, Sandmann F, Atkins KE, Robotham JV , et al. Quantifying the economic cost of antibiotic resistance and the impact of related interventions: rapid methodological review, conceptual framework and recommendations for future studies. BMC Med. (2020) 18(1):38. doi: 10.1186/s12916-020-1507-2
7. Walsh TR, Gales AC, Laxminarayan R, Dodd PC. Antimicrobial resistance: addressing a global threat to humanity. PLoS Med. (2023) 20(7):e1004264. doi: 10.1371/journal.pmed.1004264
8. Alhassan MY, Ahmad AA. Antimicrobial resistance in a changing climate: a One Health approach for adaptation and mitigation. Bull Natl ResCent. (2025) 49(1):26. doi: 10.1186/s42269-025-01318-2
9. Iskandar K, Molinier L, Hallit S, Sartelli M, Hardcastle TC, Haque M , et al. Surveillance of antimicrobial resistance in low-and middle-income countries: a scattered picture. Antimicrob Resist Infect Control. (2021) 10(1):63. doi: 10.1186/s13756-021-00931-w
10. Saeed DK, Farooqi J, Shakoor S, Hasan R. Antimicrobial resistance among GLASS priority pathogens from Pakistan: 2006–2018. BMC Infect Dis. (2021) 21(1):1231. doi: 10.1186/s12879-021-06795-0
11. Venne DM, Hartley DM, Malchione MD, Koch M, Britto AY, Goodman JL. Review and analysis of the overlapping threats of carbapenem and polymyxin resistant E. coli and Klebsiella in Africa. Antimicrob Resist Infect Control. (2023) 12(1):29. doi: 10.1186/s13756-023-01220-4
12. Ngoi ST, Chong CW, Ponnampalavanar SSLS, Tang SN, Idris N, Abdul Jabar K , et al. Genetic mechanisms and correlated risk factors of antimicrobial-resistant ESKAPEE pathogens isolated in a tertiary hospital in Malaysia. Antimicrob Resist Infect Control. (2021) 10(1):70. doi: 10.1186/s13756-021-00936-5
13. Atif M, Ihsan B, Malik I, Ahmad N, Saleem Z, Sehar A , et al. Antibiotic stewardship program in Pakistan: a multicenter qualitative study exploring medical doctors’ knowledge, perception and practices. BMC Infect Dis. (2021) 21(1):374. doi: 10.1186/s12879-021-06043-5
14. Kim HS, Kim S, Shin SJ, Park YH, Nam Y, Kim CW , et al. Gram-negative bacteria and their lipopolysaccharides in Alzheimer’s disease: pathologic roles and therapeutic implications. Transl Neurodegener. (2021) 10(1):49. doi: 10.1186/s40035-021-00273-y
15. Duffey M, Jumde RP, da Costa RM, Ropponen HK, Blasco B, Piddock LJ. Extending the potency and lifespan of antibiotics: inhibitors of gram-negative bacterial efflux pumps. ACS Infect Dis. (2024) 10(5):1458–82. doi: 10.1021/acsinfecdis.4c00091
16. Gondil VS, Subhadra B. Biofilms and their role on diseases. BMC Microbiol. (2023) 23(1):203. doi: 10.1186/s12866-023-02954-2
17. Saleem Z. AMR battle in Pakistan: from national action plans to local failures. Arch Pub Health. (2025) 83(1):1–3. doi: 10.1186/s13690-025-01568-6
18. Alhassan MY, Kabara MK, Ahmad AA, Abdulsalam J, Habib HI. Revisiting antibiotic stewardship: veterinary contributions to combating antimicrobial resistance globally. Bull Natl ResCent. (2025) 49(1):25. doi: 10.1186/s42269-025-01317-3
19. Momani S, Alyahya MS, Zayed DK, Tarif AB, Nimri OF, Alshaikh S , et al. Evaluating Jordan’s antimicrobial resistance national action plan (2018–2022) implementation: progress and recommendations. BMC Pub Health. (2025) 25(1):2718. doi: 10.1186/s12889-025-24073-5
20. Yoon YK, Kwon KT, Jeong SJ, Moon C, Kim B, Kiem S , et al. Guidelines on implementing antimicrobial stewardship programs in Korea. Infect Chemother. (2021) 53(3):617. doi: 10.3947/ic.2021.0098
21. Su LH, Chen IL, Tang YF, Lee JS, Liu JW. Increased financial burdens and lengths of stay in patients with healthcare-associated infections due to multidrug-resistant bacteria in intensive care units: a propensity-matched case-control study. PLoS One. (2020) 15(5):e0233265. doi: 10.1371/journal.pone.0233265
22. Tam-Tham H, Persaud N, Arya A. Palliative care consultation teams in long-term care: a descriptive retrospective cohort study. BMC Palliat Care. (2025) 24(1):79. doi: 10.1186/s12904-025-01716-3
23. Mazzuco S, Suhrcke M, Zanotto L. How to measure premature mortality? A proposal combining “relative” and “absolute” approaches. Popul Health Metr. (2021) 19(1):41. doi: 10.1186/s12963-021-00267-y
24. Cui P, Yang M, Hu H, Cheng C, Chen X, Shi J , et al. The impact of caregiver burden on quality of life in family caregivers of patients with advanced cancer: a moderated mediation analysis of the role of psychological distress and family resilience. BMC Pub Health. (2024) 24(1):817. doi: 10.1186/s12889-024-18321-3
25. McAtee RE, Spradley L, Tobey L, Thomasson W, Azhar G, Mercado C. Caregiver burden: caregiving workshops have a positive impact on those caring for individuals with dementia in Arkansas. J Patient Exp. (2021) 8:23743735211018085. doi: 10.1177/23743735211018085
26. Uimonen M, Kuitunen I, Paloneva J, Launonen AP, Ponkilainen V, Mattila VM. The impact of the COVID-19 pandemic on waiting times for elective surgery patients: a multicenter study. PLoS One. (2021) 16(7):e0253875. doi: 10.1371/journal.pone.0253875
27. Alshehari A, Saeed A. Strategies for improving healthcare workers’ compliance with infection control measures in intensive care units: a systematic review and meta-analysis. Intens Care Res. (2024) 4(4):201–9. doi: 10.1007/s44231-025-00077-y
28. Doleman G, De Leo A, Bloxsome D. The impact of pandemics on healthcare providers’ workloads: a scoping review. J Adv Nurs. (2023) 79(12):4434–54. doi: 10.1111/jan.15690
29. Musuka G, Machakwa J, Mano O, Iradukunda PG, Gashema P, Moyo E , et al. Antimicrobial resistance and its impact on food safety determinants along the beef value chain in sub-Saharan Africa—a scoping review. Trop Med Infect Dis. (2025) 10(3):82.
30. Hussain K, Khan MF, Ambreen G, Raza SS, Irfan S, Habib K , et al. An antibiotic stewardship program in a surgical ICU of a resource-limited country: financial impact with improved clinical outcomes. J Pharm Policy Pract. (2020) 13(1):69. doi: 10.1186/s40545-020-00272-w
31. Elias C, Ha NT, Sengvilaipaserth O, Phaychith A, Chansamouth V, Phongsavath V , et al. Antibiotic prescribing practices and antibiotic use quality indicators in Luang Prabang, Lao PDR: a point prevalence survey in a tertiary care hospital. BMC Infect Dis. (2024) 24(1):818. doi: 10.1186/s12879-024-09614-4
32. Upsher R, Dommett E, Carlisle S, Conner S, Codina G, Nobili A , et al. Improving reporting standards in quantitative educational intervention research: introducing the CLOSER and CIDER checklists. J New Approaches Educ Res. (2025) 14(1):2. doi: 10.1007/s44322-024-00022-9
33. Ahmed A, Saqlain M, Tanveer M, Blebil AQ, Dujaili JA, Hasan SS. The impact of clinical pharmacist services on patient health outcomes in Pakistan: a systematic review. BMC Health Serv Res. (2021) 21(1):859. doi: 10.1186/s12913-021-06897-0
34. Chukwu EE, Abuh D, Idigbe IE, Osuolale KA, Chuka-Ebene V, Awoderu O , et al. Implementation of antimicrobial stewardship programs: a study of prescribers’ perspective of facilitators and barriers. PLoS One. (2024) 19(1):e0297472. doi: 10.1371/journal.pone.0297472
35. Gilham EL, Pearce-Smith N, Carter V, Ashiru-Oredope D. Assessment of global antimicrobial resistance campaigns conducted to improve public awareness and antimicrobial use behaviours: a rapid systematic review. BMC Pub Health. (2024) 24(1):396. doi: 10.1186/s12889-024-17766-w
36. Patton DE, Ryan C, Hughes CM. Development of a complex community pharmacy intervention package using theory-based behaviour change techniques to improve older adults’ medication adherence. BMC Health Serv Res. (2020) 20(1):418. doi: 10.1186/s12913-020-05282-7
37. Purssell E, Gould D. Teaching health care students hand hygiene theory and skills: a systematic review. Int J Environ Health Res. (2022) 32(9):2065–73. doi: 10.1080/09603123.2021.1937580
38. Link T. Guidelines in practice: environmental cleaning. AORN J. (2021) 113(5):487–99. doi: 10.1002/aorn.13376
39. Tsioutis C, Birgand G, Bathoorn E, Deptula A, Ten Horn L, Castro-Sánchez E , et al. Education and training programmes for infection prevention and control professionals: mapping the current opportunities and local needs in European countries. Antimicrob Resist Infect Control. (2020) 9(1):183. doi: 10.1186/s13756-020-00835-1
40. Endalamaw A, Khatri RB, Mengistu TS, Erku D, Wolka E, Zewdie A , et al. A scoping review of continuous quality improvement in healthcare system: conceptualization, models and tools, barriers and facilitators, and impact. BMC Health Serv Res. (2024) 24(1):487. doi: 10.1186/s12913-024-10828-0
41. Pallares C, Hernández-Gómez C, Appel TM, Escandón K, Reyes S, Salcedo S , et al. Impact of antimicrobial stewardship programs on antibiotic consumption and antimicrobial resistance in four Colombian healthcare institutions. BMC Infect Dis. (2022) 22(1):420. doi: 10.1186/s12879-022-07410-6
© The Author(s). 2025 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.